Our blood vessels are not well suited to providing a sufficient and constant blood flow for dialysis. We have two types of blood vessels: veins and arteries. Our veins are located just beneath the skin and we can often see them with the naked eye. They can be punctured quite easily, but the blood flow in veins is too low for dialysis treatment.
In the arteries, blood flows with a higher pressure than in the veins, but they are “hidden” much deeper under the skin, and are hence much more difficult to puncture. Furthermore, arteries have a very strong pulse and high pressure, which is not ideal for dialysis treatment. Therefore we need a special blood vessel called fistula.
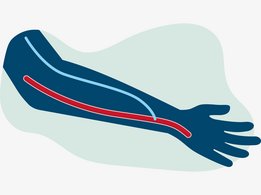
A fistula is created during a short surgical intervention by joining an artery with a vein – that is why it is called “arteriovenous”. Fistulas are usually located in the forearm. The newly created blood vessel combines the properties of arteries and veins: the blood flow and blood pressure is higher than in a vein and the blood vessel has a palpable thrill, similar to what you can feel when touching an artery.
During the maturation process the diameter of the blood vessel grows making it easier to insert a needle, and the wall thickness of the fistula increases. This “maturation process” usually takes two to six weeks. After maturation the fistula can be cannulated, as it allows a high amount of blood to flow into the extracorporeal blood circuit, enabling effective haemodialysis.

![[Translate to South Africa English:] Man checking his fistula arm](/fileadmin/_processed_/4/9/csm_fistula_care5_8dd5bab35f.jpg)


![[Translate to South Africa English:] Man washing his arm](/fileadmin/_processed_/7/b/csm_fistula_care8_77f256b4e3.jpg)
![[Translate to South Africa English:] Man riding a bicycle](/fileadmin/_processed_/c/3/csm_fistula_fcccb04a03.jpg)
![[Translate to South Africa English:] Ice and sun as symbols for extreme temperatures](/fileadmin/_processed_/7/9/csm_fistula_care10_6be8187bc0.jpg)